Plasma Cell precursor and Other Disorders
Category: Plasma Cell precursor and Other Disorders
Efficacy and Safety of Daratumumab-Based Regimens in Light Chain Amyloidosis: A Retrospective Single-Center Study
(PA-370) Efficacy and Safety of Daratumumab-Based Regimens in Light Chain Amyloidosis: A Retrospective Single-Center Study

Xinran Wang, Bachelor of Medicine, Bachelor of Surgery (MBBS)
MD Candidate
Department of Hematology, Tongji Hospital, Tongji Medical College, Huazhong University of Science and Technology
Introduction:
Light chain (AL) amyloidosis is a rare plasma cell disorder characterized by misfolded immunoglobulin light chains forming amyloid deposits in tissues and vital organs. Prognosis remains poor, particularly in patients with advanced cardiac or renal involvement. Daratumumab, an anti-CD38 monoclonal antibody, has demonstrated promising efficacy in AL, with reported response rates exceeding 80% in some studies. This retrospective analysis evaluated the real-world effectiveness and safety of various daratumumab-based regimens in patients with newly diagnosed or relapsed/refractory AL amyloidosis.
Methods:
This single-center retrospective study included patients diagnosed with AL amyloidosis who received at least three cycles of daratumumab-based treatment between May 2018 and May 2025. Regimens included combinations such as daratumumab with lenalidomide (DRd), bortezomib (DVd), pomalidomide (DPd), selinexor (SDd), ixazomib (DId), carfilzomib (DKd), or daratumumab plus dexamethasone alone (Dd). Hematologic responses were assessed per consensus criteria, and organ responses were evaluated based on cardiac and renal improvement indicators.
Results:
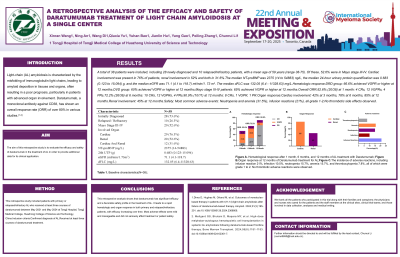
A total of 77 patients were analyzed, including 64 newly diagnosed and 13 relapsed/refractory cases. The median age was 58.5 years (range: 36–83). At baseline, 56.1% of patients were classified as Mayo stage III or IV. Cardiac involvement was present in 75.4%, renal involvement in 54.5%, and 31.5% had both.
The median baseline NT-proBNP was 2,478 ng/L, 24-hour urine protein was 0.763 g, eGFR was 75.4 mL/min/1.73 m², and difference in free light chains (dFLC) was 142.4 mg/L. After 12 months, 77.8% of patients in the DRd group and 58.9% in the DVd group achieved very good partial response (VGPR) or better. Among Mayo stage III–IV patients, 67.3% achieved VGPR or better.
Overall hematologic response rates at 1, 6, and 12 months were 60.8%, 80.7%, and 93.0%, respectively. At 12 months, 30 patients achieved complete response (CR), 33 VGPR, and 8 partial response (PR). Cardiac response rates improved from 50.8% at 3 months to 86.7% at 12 months. Among patients with renal involvement, 55.4% demonstrated renal response by month 12.
Treatment was generally well tolerated. The most frequent adverse events were neutropenia and anemia (33.4%) and infusion-related reactions (25.4%), all grade 1–2. No thromboembolic events were reported.
Conclusions: Daratumumab-based therapy is effective and well tolerated in both newly diagnosed and relapsed/refractory AL amyloidosis patients. It induces rapid and sustained hematologic responses and facilitates organ function recovery over time. Most adverse events were mild and manageable. Despite its retrospective design and single-center scope, this study adds valuable real-world evidence supporting the integration of daratumumab into treatment strategies for AL. Prospective, multicenter randomized trials are warranted to confirm these findings and establish optimal treatment protocols.
