Plasma Cell precursor and Other Disorders
Category: Plasma Cell precursor and Other Disorders
Mortality and Inpatient Hospitalization Rates Amongst Light-Chain Amyloidosis (AL) Patients During the Daratumumab Era: Results from an Analysis of US Medicare Fee-for-Service (FFS) Beneficiaries
(PA-367) Mortality and Inpatient Hospitalization Rates Amongst Light-Chain Amyloidosis (AL) Patients During the Daratumumab Era: Results from an Analysis of US Medicare Fee-for-Service (FFS) Beneficiaries

Julia Catini, PharmD, MBA (she/her/hers)
Sr. Global Medical Director
Alexion, AstraZeneca Rare Disease
Introduction: Light chain amyloidosis (AL) is a rare hematologic disorder characterized by the misfolding of immunoglobulin light chain produced by clonal plasma cells, followed by aggregation into amyloid fibrils and subsequent organ deposition, which may lead to organ dysfunction and death if not treated. Limited real-world data exist on clinical outcomes in AL patients following the approval of daratumumab as first-line therapy and its inclusion in clinical guidelines, specifically within the Medicare Fee-for-Service (FFS) population. The objective of this study is to assess mortality and inpatient hospitalization rates amongst Medicare FFS beneficiaries with AL who were newly prescribed treatment from January to December/2021.
Methods:
An observational, retrospective analysis of de-identified 100% Medicare Fee-for-Service (FFS) medical and pharmacy claims and enrollment data (Parts A/B/D) from January 1, 2020 to December 31, 2022 was performed. The index date was defined as the earliest diagnosis date (ICD-10 code) of AL within the identification window of January 1, 2021 to December 31, 2021. Patients were required to have: (1) ≥ 1 inpatient or ≥ 2 outpatient claims (≥ 30 days apart) with an ICD-10-CM diagnosis code (E85.81) for AL; (2) continuous medical and prescription insurance enrollment from 12-months pre-index through 12-months post-index (or death); (3) age ≥18 years at index, and (4) ≥1 claim for one of the following treatments within 3 months post-index: bendamustine, bortezomib, carfilzomib, cyclophosphamide, daratumumab, ixazomib, lenalidomide, melphalan, pomalidomide, or venetoclax. Patients with a prior claim for AL at baseline or any claim for stem cell transplant were excluded. Outcomes were assessed during the 12-month post-index period, including all-cause mortality and all-cause inpatient hospitalizations, stratified by daratumumab use (initiated within 3 months post-index-diagnosis).
Results:
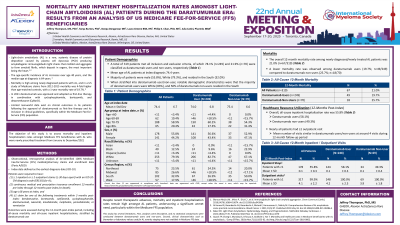
A total of 319 patients met all inclusion and exclusion criteria, of which 78.1% (n=249) and 21.9% (n=70) were classified as daratumumab users and nonusers, respectively. A majority of patients were age 70+ (79.3%; n=253), male (55.8%; n=178), White (79.3%; n=253), and resided in the South (32.0%; n=102). The overall annual mortality rate among newly diagnosed/newly treated AL patients was 21.0% (n=67/319), with a lower rate observed among daratumumab users (19.7%; n=49/249) compared to daratumumab nonusers (25.7%; n=18/70). Differences were also observed when assessing all-cause inpatient hospitalization rates during the 12-month post-index period, with 57.8% (n=144/249) and 48.6% (n=34/70) seen among daratumumab users and nonusers, respectively.
Conclusions:
Despite recent therapeutic advances, mortality and inpatient hospitalization rates remain high amongst AL patients, underscoring a significant unmet need, particularly within the Medicare FFS population.
